CMS released its 2027 Medicare Advantage and Part D Final Rule.
After last November's proposed rule, which we called the most exciting in years, the question was always how much would survive to become final. The answer: more than most expected.
CMS is simplifying and reducing the regulatory burden on distribution. For agents operating the right way, this rule removes friction without removing guardrails.
Here's what you need to know.
The 48-hour SOA rule is gone
The most significant change for brokers is one many have been waiting years for: CMS eliminated the 48-hour waiting period between when a beneficiary completes a Scope of Appointment (SOA) and when a personal marketing appointment can take place.
The SOA itself is still required but agents can now meet with a client the same day the SOA is signed.
Best practice: Collect SOAs, PTCs, and needs assessments in one step before a first meeting. Use Spark's Sources to collect digitally.
SOAs can now be collected at educational events
Brokers running educational events can now have attendees complete an SOA on the spot and move forward when they're ready. The event itself still needs to remain purely educational with no plan comparisons or sales pitches.
The 12-hour gap between educational and marketing events, during which opt-out is allowed, is also eliminated.
Best practice: Build a structured, recurring event calendar. Use our compliant Marketing Materials to promote your educational events and our branded Medicare 101 presentation to run it. Be sure to have attendees fill out a physical or digital PTC.
Marketing rules: more flexibility across the board
The TPMO disclaimer requirement has been revised.
- Instead of delivering the full disclaimer within the first 60 seconds of a client meeting, brokers now simply need to read it before discussing plan benefits. Agents can now verify identity, understand why the client is calling, and open naturally before delivering compliance language.
- The SHIP reference is also out of the required disclaimer.
Call recording retention requirements are shortened to six years for marketing and sales calls.
- This reduces the operational burden significantly for agencies managing a large volume of calls.
- Enrollment records and certain call portions remain at 10 years.
The restriction on superlatives in marketing materials relaxed
- Agents can now use superlative language ("best," "most," "top-rated") without the prior requirement to have supporting documentation on file. That said, specificity is still best: "I've helped 200 seniors in [county] find their right plan" is more persuasive than "best Medicare agent in [city]."
- The underlying rule against misleading claims still applies.
Best Practice: For TPMO disclaimers, update call scripts and website disclaimers before October 1. Remove SHIP in disclaimers. For Call Recording, update your data retention policy and communicate the change to compliance or IT before it takes effect October 1. Don't delete anything retroactively without legal review.
Part D: IRA changes are now permanent
CMS is codifying the Inflation Reduction Act's Part D restructuring into regulation. The coverage gap is officially closed. There is now a defined annual out-of-pocket cap (starting at $2,000 for 2026 and indexed annually). The Manufacturer Discount Program is formalized. Beneficiaries pay nothing in the catastrophic phase.
Stable, predictable drug costs reduce a major source of post-enrollment complaints and make the ancillary cross-sell conversation easier.
Best practice: Don't wait for AEP to talk about these Part D protections with your clients. A short note to existing clients explaining what they mean can demonstrate your knowledge and service. Use it as the opening to a broader annual review, not just a drug cost update.
Star Ratings: streamlined and refocused
CMS is removing 11 measures from the Star Ratings system, specifically administrative process measures where there's little meaningful variation between plans. What remains is a sharper focus on clinical outcomes and patient experience. A new Depression Screening and Follow-Up measure is being added, starting with the 2027 measurement year and reflected in 2029 Star Ratings.
Plans that deliver genuinely better clinical care should see their ratings reflect that more clearly. For brokers, this matters because Star Ratings drive Quality Bonus Payments, which flow into rebates and benefit richness. A more accurate ratings signal means the plans you recommend based on quality have a better chance of maintaining the benefits that earned your clients' trust.
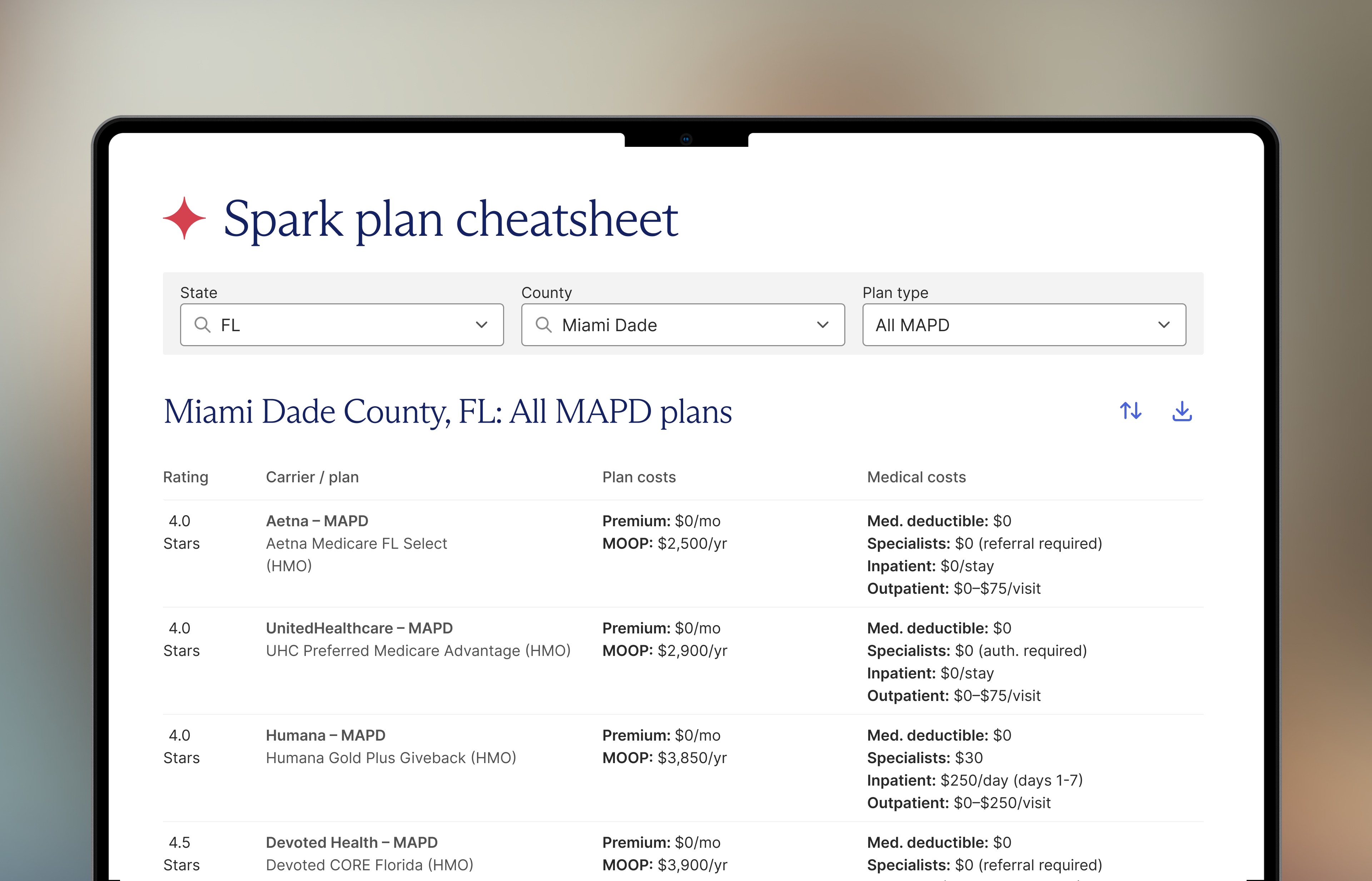
Best practice: When evaluating plans for clients, go beyond premium and benefit comparisons. A plan's Star Rating trajectory matters, especially as the new outcome-focused measure set takes hold.
Flex card: new guardrails that could save the benefit
CMS is putting guardrails around how flex cards work and how they're sold. A new point-of-sale verification system will confirm purchases qualify as covered benefits before they go through, closing the door on flex dollars being spent on unqualified items. Unused balances also won't carry over year to year.
On the marketing side, the broad unqualified statements plans have used to advertise these cards are over. Plans must now publicly post eligibility criteria, so what the benefit actually covers is visible upfront.
These changes close the gap between how flex benefits have been marketed and how they actually work. That gap has created problems for agents and members alike. Closing it is arguably what keeps this benefit viable long-term.
Best practice: Before AEP, pull each plan's posted eligibility criteria and know what the flex card actually covers. When the conversation comes up with clients, lead with what qualifies, not the dollar amount. It protects you and sets the right expectation from the start.
In summary
The 2027 final rule is the most broker-friendly CMS has put out in years. The 48-hour SOA removal alone will meaningfully change how brokers run their businesses, including fewer lost leads, smoother client conversations, and less compliance friction for agents already doing this work the right way.
The Part D codifications bring stability. The marketing rule changes stack up to a real operational improvement heading into AEP 2027.
The structural headwinds in this industry aren't going away. However, this rule reinforces something we've believed for a long time: the environment rewards brokers who have made the shift from transactional enrollments to long-term healthcare advocacy. Consistent client presence, benefit activation, and year-round engagement. That's what builds a durable book.
Key dates
June 1, 2026 - Final rule takes effect
October 1, 2026 - New marketing and communications rules apply
October 15 – Dec 7, 2026 - AEP for plan year 2027
January 1, 2027 - Plan year 2027 coverage begins




.jpeg)


.png)



















.png)






.png)



.png)
.png)



.png)

.png)
.png)
.png)
%201.png)






.png)

.png)






.png)








.png)


.png)

.png)
